A Child Is Diagnosed With Hyperthyroidism. What Finding Would the Nurse Expect to Assess?
Congenital hypothyroidism (CH) is inadequate thyroid hormone production in newborn infants.
What is Built Hypothyroidism?
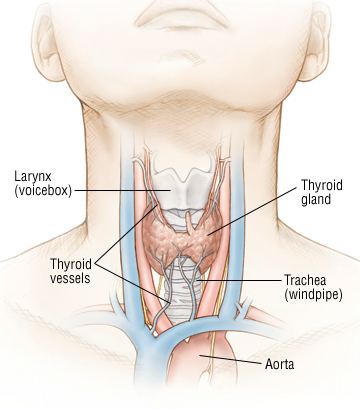
- At ane fourth dimension referred to by now unacceptable term "cretinism", congenital hypothyroidism is associated with either the congenital absenteeism of a thyroid gland or the inability of the thyroid gland to secrete thyroid hormone.
- Information technology can occur because of an anatomic defect in the gland, an inborn fault of thyroid metabolism, or iodine deficiency.
- Lower TSH screening cutoffs may likewise be driving this increment in diagnosis, although altered ethnicities of the screened population, increased multiple and premature births, and iodine status are contributing factors.
- In the 1920s, adequate dietary intake of iodine was establish to prevent endemic goiter and cretinism.
- The term sporadic cretinism was initially used to depict the random occurrence of cretinism in nonendemic areas; the cause of these abnormalities was identified as nonfunctioning or absent thyroid glands.
Pathophysiology
The thyroid gland develops from the buccopharyngeal cavity between iv and 10 weeks' gestation.
- The thyroid arises from the fourth branchial pouches and ultimately ends upwardly equally a bilobed organ in the neck.
- Past ten-11 weeks' gestation, the fetal thyroid is capable of producing thyroid hormone; by 18-20 weeks' gestation, blood levels of T4 accept reached term levels.
- The thyroid gland uses tyrosine and iodine to manufacture T4 and triiodothyronine (T3).
- Inborn errors of thyroid metabolism can result in congenital hypothyroidism in children with anatomically normal thyroid glands.
- T4 is the primary thyronine produced by the thyroid gland; but 10-twoscore% of circulating T3 is released from the thyroid gland.
- T3 is the principal mediator of the biologic effects of thyroid hormone and does so by interacting with a specific nuclear receptor; receptor abnormalities can result in thyroid hormone resistance.
- The major carrier proteins for circulating thyroid hormones are thyroid-binding globulin (TBG), thyroid-bounden prealbumin (TBPA), and albumin.
- Infants born with low levels of TBG, as in congenital TBG deficiency, have low total T4 levels just are physiologically normal; familial congenital TBG deficiency can occur every bit an 10-linked recessive or autosomal recessive condition.
- The most critical period for the outcome of thyroid hormone on encephalon development is the first few months of life.
Statistics and Incidences
CH is the most mutual neonatal endocrine disorder, and historically, thyroid dysgenesis was thought to business relationship for approximately fourscore% of cases.
- An increased incidence of congenital hypothyroidism is observed in twins; twin births are approximately 12 times as probable to have built hypothyroidism as singletons.
- Usually, only ane twin is hypothyroid, merely a common in-utero exposure tin can cause hypothyroidism in both.
- Most studies of congenital hypothyroidism propose a female-to-male person ratio of a 2:1; Devos et al showed that much of the discrepancy is accounted for by infants with thyroid ectopy.
- In central Africa, where iodine deficiency occurs along with excess dietary cyanate from cassava (Manihot esculenta), as many every bit x% of newborns may have both low cord blood T4 concentration and TSH concentrations over 100 mU/50.
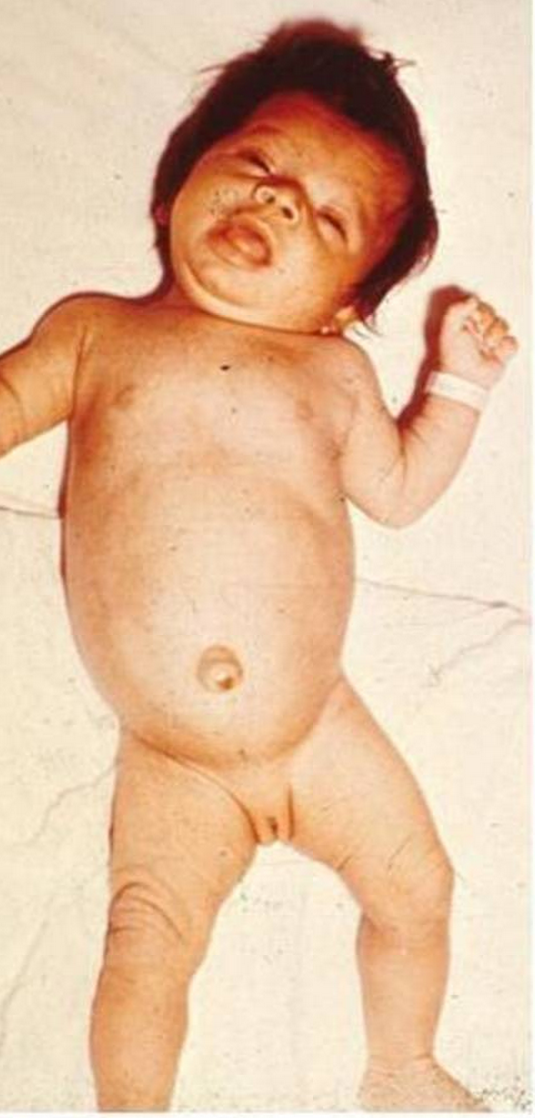
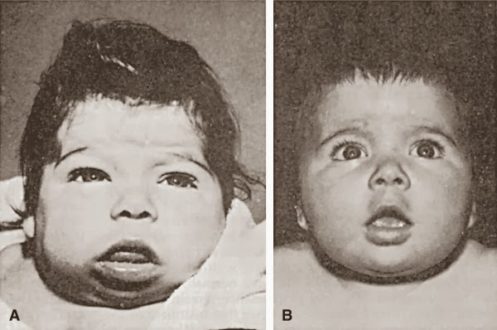
Clinical Manifestations
The physical findings of hypothyroidism may or may not be present at nascence.
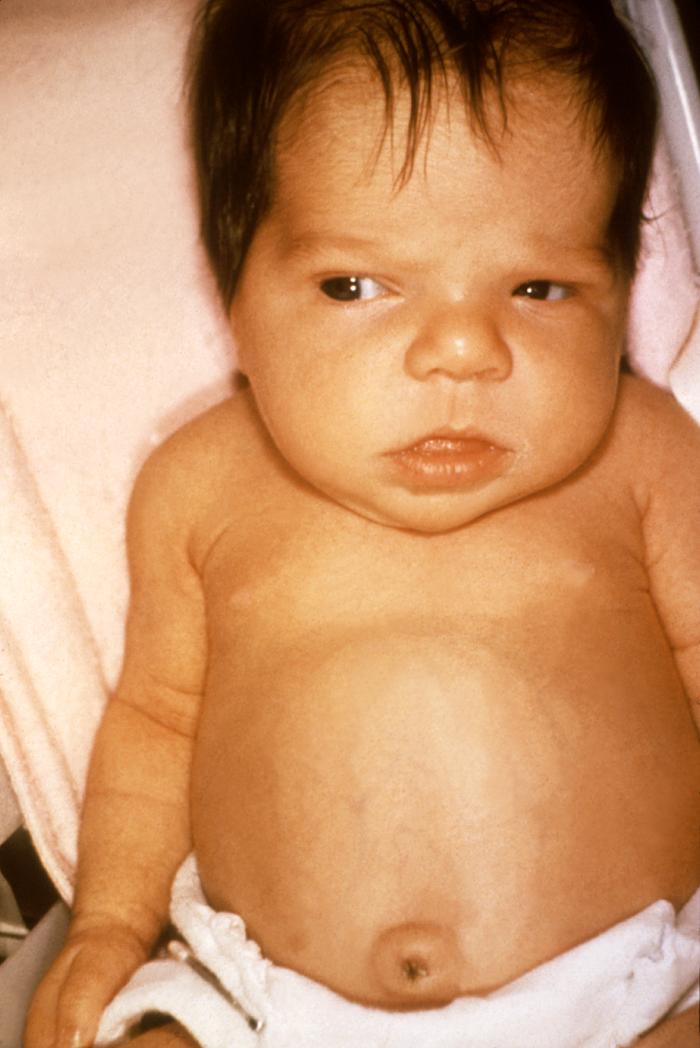
- Decreased activeness. Frequently, affected infants are described equally "proficient babies" considering they rarely cry and they slumber almost of the fourth dimension.
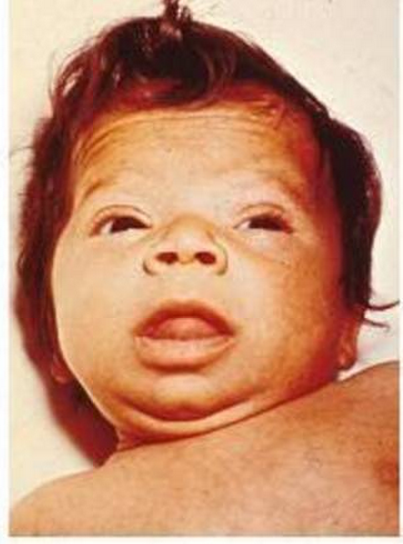
- Large anterior fontanelle. A big anterior fontanelle is mostly found in infants with CH, with delayed closure.
- Poor feeding and weight gain. A child with CH more often than not sleeps and rarely feeds, resulting in poor weight gain.
- Small stature or poor growth. There is a filibuster in the development of children with CH, with poor growth as one of the findings.
- Jaundice. The xanthous coloration of the skin and sclera in newborns with jaundice is the event of accumulation of unconjugated bilirubin.
Assessment and Diagnostic Findings
Diagnosis of master hypothyroidism is confirmed by demonstrating decreased levels of serum thyroid hormone (total or free T4) and elevated levels of thyroid-stimulating hormone (TSH).
- Newborn screening. Screening for congenital hypothyroidism is recommended when a baby is 3 days former; testing should be performed earlier belch or within 7 days of birth; false-positive TSH elevations may be establish in specimens collected at 24-48 hours after nativity, and false-negative results may be found in critically ill newborns or post-transfusion infants.
- T4 levels. Low or depression-normal serum total T4 levels in the setting of a serum TSH within the reference range suggests TBG deficiency; this congenital disorder causes no pathologic outcome; however, it should be recognized to avoid unnecessary thyroid hormone assistants.
- Ultrasonography and scintigraphy. Ultrasound and thyroid scintigraphy help decide the anatomy and function of the thyroid gland as well as the etiology of congential hypothyroidism; ultrasound lacks sensitivity for detecting small ectopic glands but is the gold standard for measuring thyroid dimensions; scintigraphy (using technetium-99m or iodine-123) provides an etiologic diagnosis in near cases and tin aid in distinguishing congenital hypothyroidism from transient hyperthyrotropinemia.
- Radiography.A lateral radiograph of the knee may be obtained to look for the distal femoral epiphysis; this ossification centre appears at about 36 weeks' gestation; its absence in a term or postterm infant indicates prenatal effects of hypothyroidism.
Medical Management
The thyroid hormone must be replaced equally before long equally the diagnosis is made. The goal of treatment in built hypothyroidism is to right hypothyroidism and ensure normal growth and neuropsychological evolution.
- Levothyroxine. Only levothyroxine is recommended for handling; it has been established as condom, effective, inexpensive, easily administered, and easily monitored.
- Nutrition. Dietary iodide supplementation in iodine-deficient areas can forestall owned cretinism simply does not have a major event on desultory congenital hypothyroidism; soy-based formulas may decrease the absorption of levothyroxine; this is non a contraindication to their use, even in infants with built hypothyroidism; switching an babe from a milk-based formula to a soy-based formula may increase the dose of thyroid hormone needed to maintain a euthyroid status.
Pharmacologic Management
The drug of choice for CH is simply Levothyroxine.
- Thyroid hormones. These agents are administered to supplement thyroid hormone in patients with hypothyroidism. Levothyroxine is the preferred class of thyroid hormone replacement in all patients with hypothyroidism.
Nursing Management
Nursing care of a kid with built hypothyroidism include the post-obit:
Nursing Assessment
Assessment of a child with congenital hypothyroidism include:

- History. Family unit history should be carefully reviewed for information about similarly affected infants or family unit members with unexplained mental retardation; maternal history of a thyroid disorder and mode of treatment, whether earlier or during pregnancy, can occasionally provide the etiology of the infant's trouble.
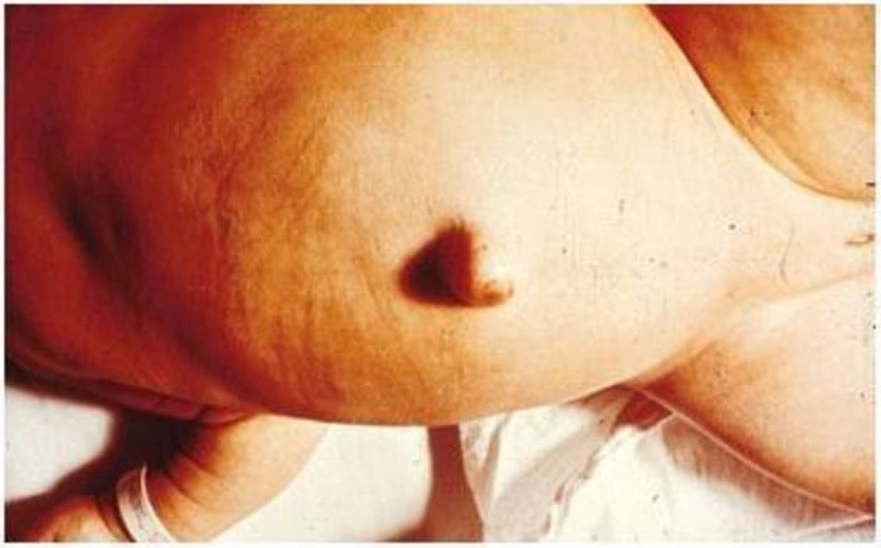
- Physical exam. Concrete exam may evidence signs of coarse facial features, macroglossia, large fontanelles, umbilical hernia, developmental delay, pallor, myxedema, and goiter.
Nursing Diagnosis
Based on the cess data, the major nursing diagnosis for congenital hypothyroidism are:
- Imbalanced nutrition: more than body requirements related to greater intake than metabolic needs as evidenced past hypotonia or decreased activity level.
- Deficient knowledge related to lack of exposure to hypothyroidism and unfamiliarity with data sources.
- Fatigue related to impaired metabolic state.
Nursing Care Planning and Goals
Main Commodity: 3 Hypothyroidism Nursing Care Plans
The major nursing intendance planning goals for congenital hypothyroidism are:
- Customer will maintain a stable weight and takes in necessary nutrients.
- Family members/caregivers will verbalize correct information about hypothyroidism and taking thyroid hormone replacement.
- Family members/caregivers volition identify basis of fatigue and individual areas of control.
- Family unit members/caregivers will verbalize reduction of fatigue and increased ability to complete desired activities.
Nursing Interventions
The nursing interventions are:
- Maintain a stable weight. Educate the client and family regarding body weight changes in hypothyroidism; interact with a dietician to determine client's caloric needs; encourage the intake of foods rich in fiber; encourage a low-cholesterol, low-calorie, depression-saturated-fat diet.
- Learn more than about the disease. Provide data about hypothyroidism; educate the client and family regarding thyroid hormones; emphasize the importance of rest periods.
- Reduce fatigue. Note daily free energy patterns; plan care to allow individually adequate balance periods; schedule activities for periods when the client has the most free energy; promote an environment conducive to relieve fatigue.
Evaluation
Goals are met as evidenced past:
- Customer maintained a stable weight and takes in necessary nutrients.
- Family unit members/caregivers verbalized correct information about hypothyroidism and taking thyroid hormone replacement.
- Family members/caregivers identified ground of fatigue and individual areas of command.
- Family members/caregivers verbalized reduction of fatigue and increased power to complete desired activities.
Documentation Guidelines
Documentation in a kid with congenital hypothyroidism include:
- Individual findings, including factors affecting, interactions, nature of social exchanges, specifics of individual behavior.
- Intake and output.
- Cultural and religious beliefs, and expectations.
- Programme of care.
- Pedagogy plan.
- Responses to interventions, educational activity, and actions performed.
- Attainment or progress toward desired outcome.
Exercise Quiz: Congenital Hypothyroidism
Hither'due south a 5-particular quiz for Built Hypothyroidism study guide. Please visit our nursing examination banking company page for more NCLEX practice questions.
1. The physician has discussed the demand for medication with the parents of an babe with congenital hypothyroidism. The nurse tin can reinforce the physician's pedagogy by telling the parents that:
A. The medication will be needed only during times of rapid growth.
B. The medication is given one fourth dimension daily every other day.
C. The medication schedule tin can be bundled to allow for drug holidays.
D. The medication will be needed throughout the child's lifetime.
1. Respond: D. The medication volition be needed throughout the kid's lifetime.
- Option D: The medication will be needed throughout the child's lifetime.
- Options A, C, D: Answers A, C, and D contain inaccurate statements; therefore, they are incorrect.
2. Ruby is receiving thyroid replacement therapy develops the flu and forgets to take her thyroid replacement medicine. The nurse understands that skipping this medication will put the client at take a chance for developing which of the post-obit life-threatening complications?
A. Exophthalmos
B. Thyroid storm
C. Myxedema coma
D. Tibial myxedema
ii. Answer: C. Myxedema coma.
- Option C: Myxedema blackout, severe hypothyroidism, is a life-threatening condition that may develop if thyroid replacement medication isn't taken.
- Option A: Exophthalmos, protrusion of the eyeballs, is seen with hyperthyroidism.
- Option B: Thyroid storm is life-threatening but is caused past severe hyperthyroidism.
- Pick D: Tibial myxedema, peripheral mucinous edema involving the lower leg, is associated with hypothyroidism just isn't life-threatening.
3. The physician orders laboratory tests to confirm congenital hyperthyroidism in a female client with archetype signs and symptoms of this disorder. Which examination upshot would confirm the diagnosis?
A. No increase in the thyroid-stimulating hormone (TSH) level after xxx minutes during the TSH stimulation test.
B. A decreased TSH level.
C. An increase in the TSH level after xxx minutes during the TSH stimulation test.
D. Beneath-normal levels of serum triiodothyronine (T3) and serum thyroxine (T4) as detected by radioimmunoassay.
3. Answer: A. No increment in the thyroid-stimulating hormone (TSH) level after 30 minutes during the TSH stimulation test.
- Option A: In the TSH examination, failure of the TSH level to rise after 30 minutes confirms hyperthyroidism.
- Option B: A decreased TSH level indicates a pituitary deficiency of this hormone.
- Option D: Below-normal levels of T3 and T4, every bit detected by radioimmunoassay, signal hypothyroidism. A below-normal T4 level also occurs in malnutrition and liver disease and may result from administration of phenytoin and certain other drugs.
iv. A newborn has been diagnosed with hypothyroidism. In discussing the status and treatment with the family, the nurse should emphasize:
A. They tin look the child volition be mentally retarded.
B. Assistants of thyroid hormone will preclude issues.
C. This rare problem is ever hereditary.
D. Physical growth/development will exist delayed.
4. Answer: B. Administration of thyroid hormone will forbid problems.
- Option B: Early identification and continued treatment with hormone replacement correct this status.
- Option A: With early treatment, mental retardation could exist prevented.
- Option C: Congenital hypothyroidism is not hereditary.
- Option D: There could be a delay in physical growth and development with tardily diagnosis.
five. A nurse is giving discharge instructions to the caregivers of a patient who is taking levothyroxine (Synthroid). The nurse instruct the client to notify the physician if which of the following occurs?
A. Common cold intolerance
B. Tremors
C. Coarse, dry pilus
D. Muscle cramps
5. Respond: B. Tremors
- Option B:Excessive doses of levothyroxine can produce signs and symptoms of hyperthyroidism which includes estrus tolerance, tremors, nervousness, tachycardia, chest pain, hyperthermia, and insomnia.
- Options A, C, D: Options A, C, and D are signs of hypothyroidism.
Source: https://nurseslabs.com/congenital-hypothyroidism/
0 Response to "A Child Is Diagnosed With Hyperthyroidism. What Finding Would the Nurse Expect to Assess?"
Post a Comment